Cord Knots During Pregnancy
The term “true knot of the umbilical cord” (TKUC) refers to the formation of a knot during pregnancy, while “false knot” describes a bulge in the cord resulting from excessive Wharton’s jelly or looping of cord vessels. True umbilical cord knots are significant as they can lead to various negative perinatal outcomes, such as small for gestational age (SGA) fetuses, low Apgar scores at birth, fetal hypoxia, and even fetal death.
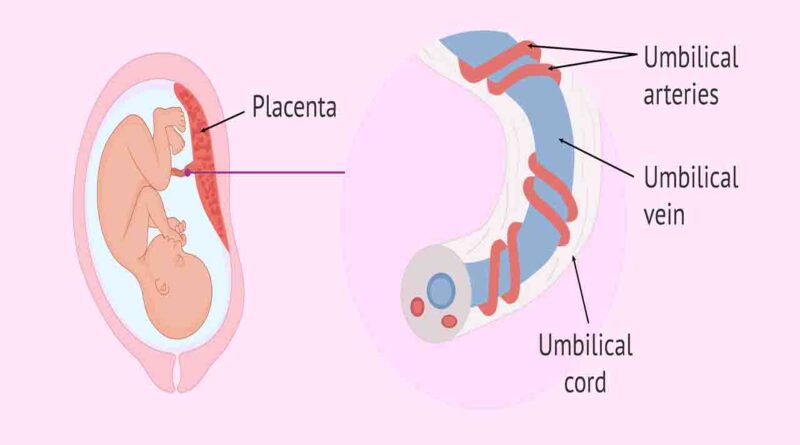
Given that the umbilical cord is the source of fetal blood supply, any defect in the cord can profoundly impact fetal well-being. Factors like increased cord length, polyhydramnios, male gender, amniocentesis, monoamniotic twins, grand multiparity, and small fetuses can predispose to TKUC. The risk of fetal death from TKUC is up to four times higher than that from other causes, exerting a broad spectrum of adverse effects on both pregnancy and labor.
What are umbilical cord knots?
A cord knot is precisely what the term implies—a knot in the baby’s umbilical cord. Some knots develop during pregnancy as the baby moves and rotates within the amniotic sac, while others may form during delivery.
Wharton’s jelly, a substance that surrounds the crucial blood vessels of the cord, acts as a cushion, providing protection even if the cord becomes knotted. This implies that the chances are favorable for a “true” tight knot not to occur.
As long as the knot remains loose, it poses no harm to the baby. However, if the knot tightens, it has the potential to impede the circulation of blood from the placenta to the baby, leading to oxygen deprivation. Such a complication is more likely to occur during the baby’s descent through the birth canal, although such cases are rare.
How common are umbilical cord knots?
Keeping an eye out for potential signs of an umbilical cord knot is prudent, allowing you to promptly inform your healthcare practitioner; however, such knots are relatively uncommon, happening in approximately one out of every hundred pregnancies.
More prevalent than knots are nuchal loops, the technical designation for when the umbilical cord encircles the baby’s neck. Nuchal loops, also referred to as nuchal cords, are observed in about 20 percent of all pregnancies but seldom pose significant risks to the baby.
Who is most at risk for umbilical cord knots?
Babies with long umbilical cords and those classified as small for their gestational age face an elevated risk of developing true knots in the umbilical cord. Several factors contribute to this increased susceptibility:
-
Long Umbilical Cords:
- Increased Mobility: A longer umbilical cord provides greater mobility for the baby within the amniotic sac. As the baby moves and turns, especially during the later stages of pregnancy, the likelihood of the cord forming knots increases.
- Twisting and Coiling: The extended length of the cord allows for more twisting and coiling, providing ample opportunities for knots to develop during the baby’s movements.
-
Small for Gestational Age (SGA) Babies:
- Reduced Amniotic Fluid: SGA babies are often associated with reduced amniotic fluid levels. With less amniotic fluid, the baby may have less room to move freely, increasing the chances of the umbilical cord becoming knotted.
- Intrauterine Constraint: In cases of fetal growth restriction, where the baby is smaller than expected for its gestational age, there may be limited space within the uterus. This constraint can lead to increased interactions between the baby and the umbilical cord, contributing to the formation of knots.
-
Combination of Factors:
- Long Cord and SGA Combination: The risk is further compounded when both factors—long umbilical cords and being small for gestational age—are present simultaneously. A lengthy cord combined with a restricted intrauterine environment can create conditions conducive to the development of true knots.
It is essential for healthcare providers to be aware of these risk factors during prenatal care. Regular monitoring, including ultrasound assessments, can help identify these conditions early on and allow for appropriate management to mitigate potential complications associated with true umbilical cord knots.
What are the symptoms of cord knots?
The primary indicator of a cord knot is diminished fetal activity, particularly notable after the 37th week of pregnancy. In cases where the knot forms during labor, an abnormal fetal heart rate can be detected through the use of a fetal monitor.
Preventing the occurrence of a knotted umbilical cord is not within one’s control. However, expectant mothers can play an active role in monitoring their baby’s well-being, particularly in the later stages of pregnancy. Regular kick counts, where mothers keep track of their baby’s movements, can provide valuable insights. If there is any observed deviation from the usual pattern of fetal activity, promptly notifying the healthcare practitioner is crucial.
In the event that a loosely formed knot tightens during delivery, the healthcare provider will be able to identify the associated drop in the baby’s heart rate. Subsequently, appropriate decisions will be made to ensure the safe delivery of the baby into the world. Immediate delivery, often through a Cesarean section (C-section), is frequently the preferred course of action to safeguard the well-being of both the mother and the baby.
References
- March of Dimes, Umbilical Cord Conditions Opens a new window, June 2016.
- National Institutes of Health, National Library of Medicine, Risk factors associated with true knots of the umbilical cord Opens a new window, September 2001.
- American Journal of Obstetrics & Gynecology, Multiple nuchal cord loops and neonatal outcomes Opens a new window, January 2018.
- WhatToExpect.com, Hydramnios During Pregnancy, December 2020.
- Military Medicine, True knot of the umbilical cord: A report of 13 cases, August 2007.
- National Institutes of Health, National Library of Medicine, Nuchal cord and its complications, December 2017.
See this also –
- Chorioamnionitis During Pregnancy | Intrauterine infection
- Implantation Bleeding: When It Happens and What It Looks Like